And the physician who prescribed therapy isn't in the conversation.
35–40% of specialty prescriptions are abandoned before the first fill. Of those who start, half discontinue within a year.
Not because the therapy doesn't work. Because Reddit, TikTok, AI chatbots, and Google are making the decision for them. The physician's voice vanishes the moment patients leave the exam room.
Within 72 hours of a prescription, these sources make the treatment START decision for the patient. For those who do start, these same sources drive discontinuation at Month 1, Month 3, and Month 6. The physician's voice is absent at every critical moment.
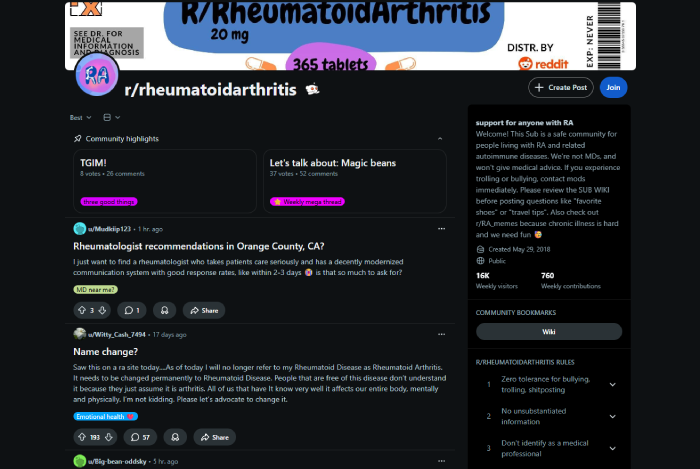


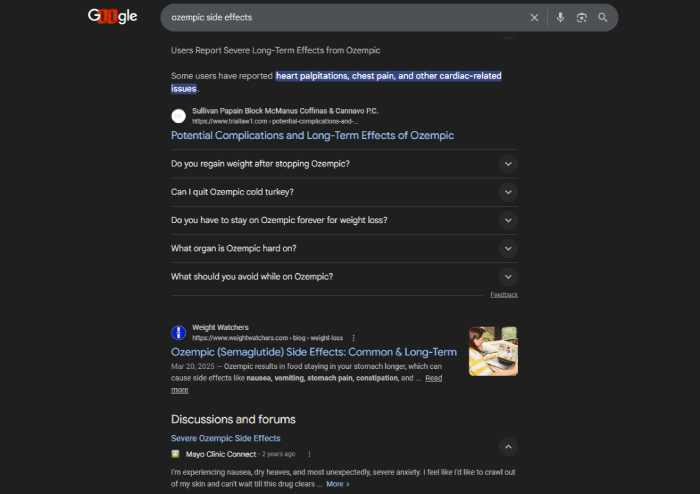
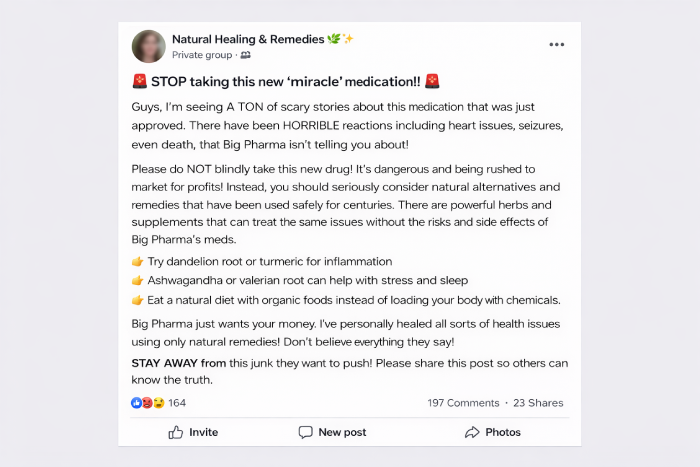
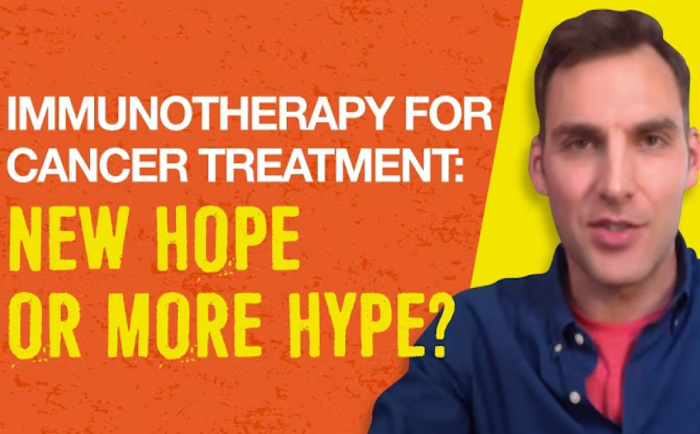
Non-medical social media influencers with millions of followers are intercepting patients between the prescription and the pharmacy counter. They have more reach than every hub call center combined. They show up when the physician doesn't. And they tell patients not to start.



This isn't abstract. The confusion crisis destroys value at two points: patients who never fill the first prescription (failed starts), and patients who start but discontinue within 6 months (lost adherence). For a single oncology product, the combined impact is staggering.
Consider a branded oncology therapy (immunotherapy, targeted therapy, or novel combination regimen) with an average annual revenue per patient of $80,000. The brand writes 10,000 new prescriptions per quarter through its oncology network.
At a 40% abandonment rate, 4,000 patients per quarter never start. They never fill the first prescription. That's the first revenue collapse. These patients left their oncologist's office intending to begin treatment, and within 72 hours decided not to, because Reddit, TikTok, Facebook groups, and ChatGPT reached them before the hub call center did.
Of the 6,000 who do start, another 20% discontinue within 6 months, driven by side-effect fear amplified by the same misinformation sources, compounded by the absence of the physician's reassuring voice during the most difficult weeks of treatment. The hub CRM logs "patient non-adherent." The revenue is already gone at two distinct failure points: starts, then adherence.
Hub services, nurse educators, copay programs, adherence apps. The infrastructure exists. But 59% of patients don't know their support program exists, and 42% of prescribers don't mention it.
The gap isn't program design. It's the silence between prescription and program: the 72 hours where misinformation fills the void. That gap is where Hoot operates.
One is ignored. One is watched within minutes.
Not listened to
This is the window where treatment starts are won or lost. The physician's voice is absent. Misinformation fills the gap. By hour 72, the start decision is made, and for 35–40%, it's a decision not to fill.
Oncology, rare disease, and medical device patients face the most extreme emotional and informational barriers. The misinformation is more dangerous. The stakes are higher. The physician's voice matters more.

Cancer patients face extreme emotional vulnerability combined with complex protocols: immunotherapy, CAR-T, targeted therapy, radiation, surgical oncology. Facebook groups actively promote treatment abandonment with alt-medicine claims.

Small patient populations, ultra-specialized prescribers, gene therapy and cell therapy protocols that patients can barely pronounce, let alone understand. 84% of providers report difficulty starting patients on specialty medications.

Orthopedic implants, cardiac devices, surgical robotics. Patients sign consent forms they don't comprehend. YouTube videos about "device failures" and "class action lawsuits" create post-surgical anxiety and non-compliance with rehab protocols.
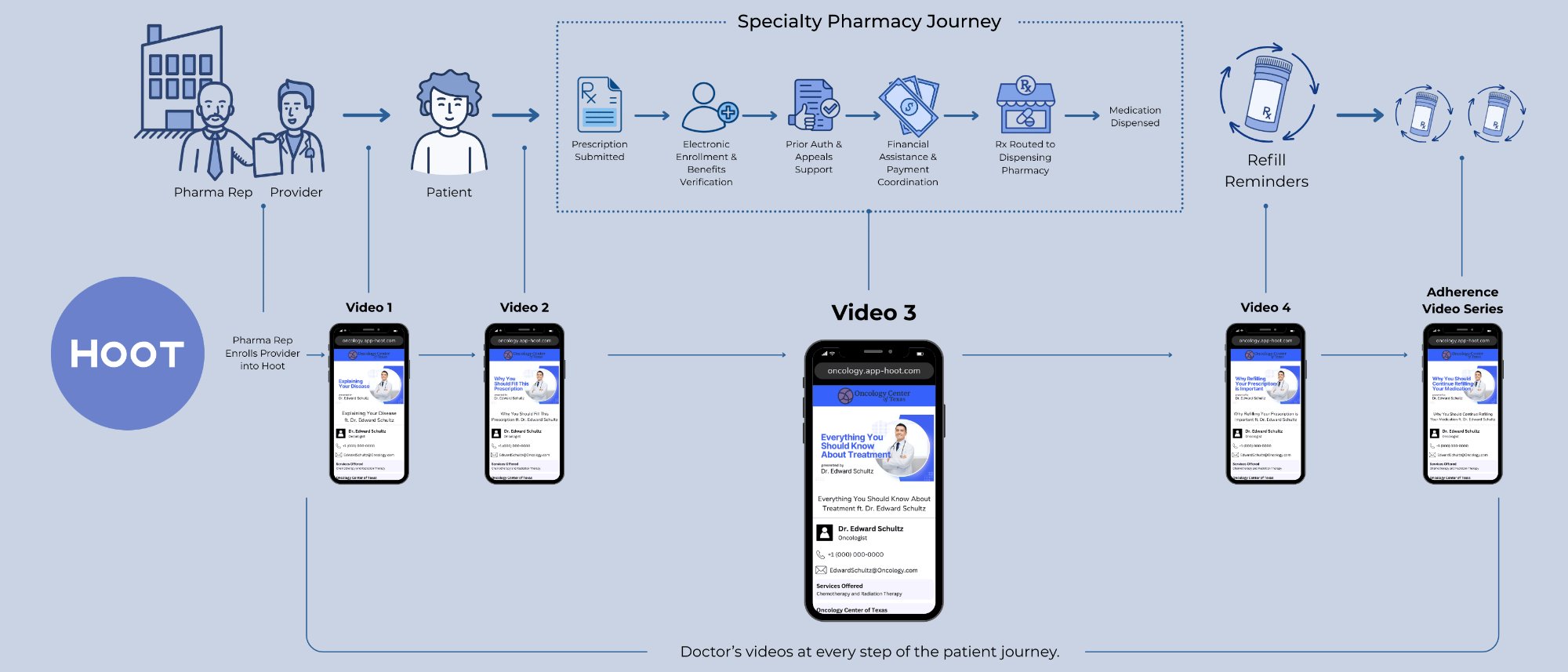
Hoot doesn't replace hub services, specialty pharmacy operations, or patient support programs. It adds the one thing they're missing: the prescribing physician's voice at every step of the patient journey, from enrollment through adherence.
Misinformation, AI hallucinations, and the $5B support program failure. The complete research brief.
Download the ReportSynthesizes data from Tufts CSDD, IQVIA, J.D. Power, and peer-reviewed adherence studies across oncology, rare disease, immunology, and med device.
Core thesis: the missing link in patient support isn't the program. It's the messenger. When the physician's voice disappears, Reddit, TikTok, and AI chatbots fill the void.

The systemic failure of patient education across oncology, rare disease, med device, and complex therapies, where patients make treatment decisions based on Reddit, TikTok, ChatGPT hallucinations, and Google fear rather than their physician's voice. Despite $5B in annual support programs, only 3% of patients use them.
Patients increasingly ask ChatGPT, Google AI Overviews, and other AI tools about their medications. These tools generate confident, authoritative-sounding medical information that is frequently inaccurate, fabricating statistics, misattributing clinical trial data, and providing misleading risk assessments that patients accept as fact because the output "sounds" clinical.
Oncology patients face life-or-death treatment decisions under extreme emotional duress, making them disproportionately susceptible to conspiracy theories and alternative medicine claims. Rare disease patients navigate ultra-specialized therapies with minimal peer support, leaving them isolated with unverified online sources. Both populations need the physician's voice most, and lose it fastest.
The prescribing physician's voice is trusted by 92% of patients, more than any other source. Hoot delivers that voice via SMS at 98% open rates during the 72-hour hesitation window when misinformation peaks. A 90-second video from the prescribing physician carries more emotional authority than every Reddit thread, TikTok video, and ChatGPT output combined.
The Patient Confusion Audit maps the specific misinformation sources, hesitation triggers, and trust gaps that prevent patients from starting therapy, and the adherence failure points that cause those who start to discontinue. Includes a revenue recovery projection for both.